WASHINGTON, APRIL 14, 2026 —
Key Takeaways
- Artificial intelligence is now outperforming human physicians in detecting breast cancer, lung nodules, diabetic retinopathy, and early Alzheimer’s markers across multiple peer-reviewed studies — while generating fewer false positives and dramatically shorter diagnostic times.
- The FDA has issued breakthrough device designations to more than 1,200 AI-powered medical tools since 2016, with the pace of approvals accelerating sharply in 2025 and 2026 as the technology matures from detection-only to full clinical reasoning.
- The global AI healthcare market — worth approximately $26.6 billion in 2024 — is projected to reach $187 billion by 2030, making it one of the fastest-growing technology sectors in the world and one with direct, personal consequences for every American’s healthcare access and costs.
Something fundamental is changing in American medicine — and it is happening faster than most patients, doctors, or policymakers realize. Artificial intelligence is no longer a research curiosity or a hospital pilot program. In 2026, it is an operational tool embedded in radiology departments, cancer screening workflows, cardiology clinics, and early dementia detection programs across the country. And the results are beginning to rewrite what was previously believed possible in early disease detection.
The shift carries profound implications not just for how doctors work — but for how many lives are saved, how early conditions are caught before they become catastrophic, and ultimately how much American healthcare costs.
What AI Can Now Do That Doctors Simply Cannot
The most dramatic advances in AI healthcare in 2026 are not in areas where machines simply do what doctors do, but faster. They are in areas where machines detect patterns that human eyes and brains physically cannot — patterns spread across millions of data points, imaging studies, genomic sequences, and patient histories simultaneously.
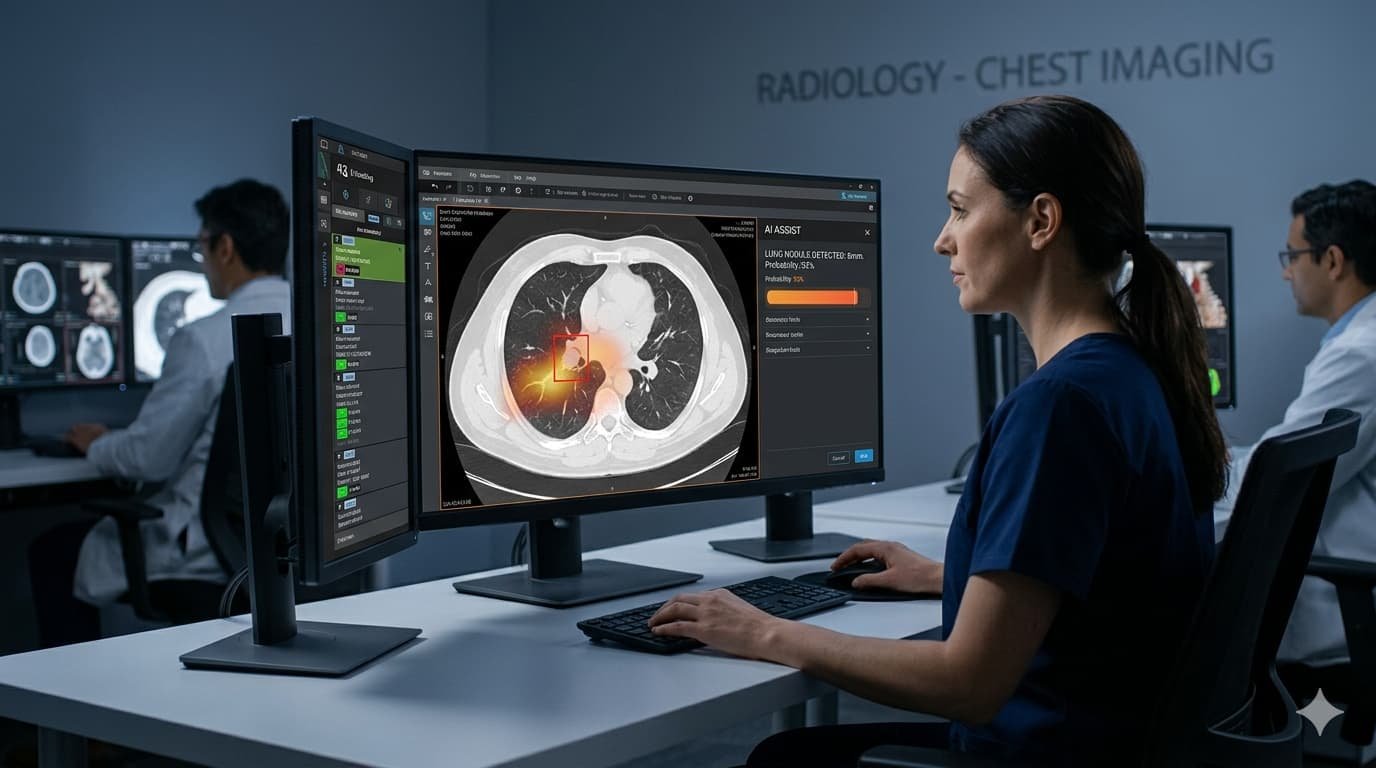
In radiology, AI triage systems now automatically sort imaging scans by urgency, ensuring that the most critical cases reach specialists first rather than sitting in a queue behind routine studies. When radiologists work alongside AI tools, detection rates for breast cancer, lung nodules, and bone fractures increase significantly while false positives — the scans that send patients through unnecessary biopsies, anxiety, and follow-up costs — decrease substantially.
In cancer care, AI systems can now compare a new tumor scan against years of prior imaging in seconds — work that previously required a radiologist to manually pull and review historical films. The ability to track tiny changes in a lesion over time with machine precision has already changed surgical planning in multiple cancer types.
The Alzheimer’s front is perhaps the most significant. Blood-based biomarker tests analyzed by AI can now detect markers of cognitive decline years before the first symptoms appear. One system built by researchers at the University of Michigan can interpret brain MRI scans in seconds, accurately identifying a wide range of neurological conditions and flagging which cases require urgent intervention. For a disease where timing determines everything — and where treatment options are most effective in the earliest stages — catching Alzheimer’s years earlier is not a marginal improvement. It is a transformative one.
How This Is Already Changing Hospitals Near You
The adoption curve for AI healthcare tools in the United States accelerated sharply in 2025 and 2026, driven by three converging forces: a physician burnout crisis that has pushed hospitals to seek anything that reduces administrative load, a reimbursement shift toward value-based care that rewards outcomes over volume, and AI tools that have finally crossed the accuracy threshold required for clinical trust.
The most widely deployed AI application in hospitals right now is not diagnostic — it is documentation. Healthcare workers currently spend up to 70% of their time on administrative tasks, with clinical note-writing consuming enormous amounts of physician hours that could be spent with patients. AI-powered ambient listening systems — microphones that sit in exam rooms and automatically transcribe and structure clinical documentation — are now deployed across thousands of clinics nationwide.
| AI Healthcare Applications Now in Active Use | Impact |
|---|---|
| Radiology triage and cancer detection | Faster diagnosis, fewer missed tumors |
| Ambient clinical documentation | 15–20 physician hours saved per week |
| Sepsis prediction | Detection hours before symptoms, saving lives |
| Alzheimer’s early detection via blood biomarkers | Years earlier diagnosis window |
| Drug interaction checking at point of care | Reduced medication errors |
| Clinical trial matching | More patients enrolled faster |
| Personalized treatment selection | Matching patients to therapies by genetics |
For patients, the most visible near-term change will come in early disease detection and speed. Waiting days for imaging results or pathology reports will increasingly be replaced by same-day or same-hour turnaround as AI handles routine analysis. Rural patients — who have historically faced massive disparities in access to specialist expertise — will gain access to AI-powered diagnostic tools that deliver specialist-level interpretation regardless of geography.
The Problems That Still Need to Be Solved
The advances are real. So are the risks. AI diagnostic tools are trained on data — and if that data contains historical biases in how diseases were documented, diagnosed, or treated across different demographics, the AI will inherit those biases. Multiple studies have found that early AI dermatology tools performed significantly worse on darker skin tones because training datasets were overwhelmingly composed of lighter-skinned patients.
Transparency is a second major challenge. Many of the most powerful AI diagnostic systems operate as what engineers call “black boxes” — they produce a recommendation without being able to explain in human-understandable terms exactly why they reached it. Physicians and patients are increasingly unwilling to accept consequential medical recommendations without explainability, and regulators are beginning to require it.
The FDA’s accelerating pace of breakthrough device approvals in the AI space reflects both the technology’s genuine promise and the institutional pressure not to let regulatory caution slow life-saving tools. Balancing those two imperatives — moving fast enough to save lives, carefully enough not to deploy biased or unreliable systems — is the defining challenge for American healthcare AI in the years ahead.
Why This Matters
Every American who gets a mammogram, a chest CT, or a blood panel in the next five years is increasingly likely to have that test analyzed with some degree of AI assistance. The question is not whether AI enters your healthcare — it already has in many hospitals. The question is whether it arrives transparently, equitably, and in ways that genuinely serve patients rather than primarily reduce hospital costs.
The potential upside is enormous. McKinsey projects AI could increase U.S. healthcare productivity by 1.8% to 3.2% annually — equivalent to $150 billion to $260 billion in system-wide cost savings per year. If even half that potential is realized and distributed to patients through lower costs and earlier interventions, AI may represent the most significant improvement in American healthcare access since Medicare itself.