CLEVELAND, MARCH 23, 2026 —
Key Takeaways
- A Cleveland Clinic study of nearly 8,000 patients found that stopping Ozempic or Mounjaro does not typically cause major weight regain in real-world settings — contradicting what earlier clinical trials suggested
- Obesity patients who stopped GLP-1 drugs had lost an average of 8.4% of body weight before quitting — and regained only 0.5% one year later
- The key to avoiding rebound weight gain is what patients do next — those who switched medications, restarted treatment, or committed to structured lifestyle support kept most of their results
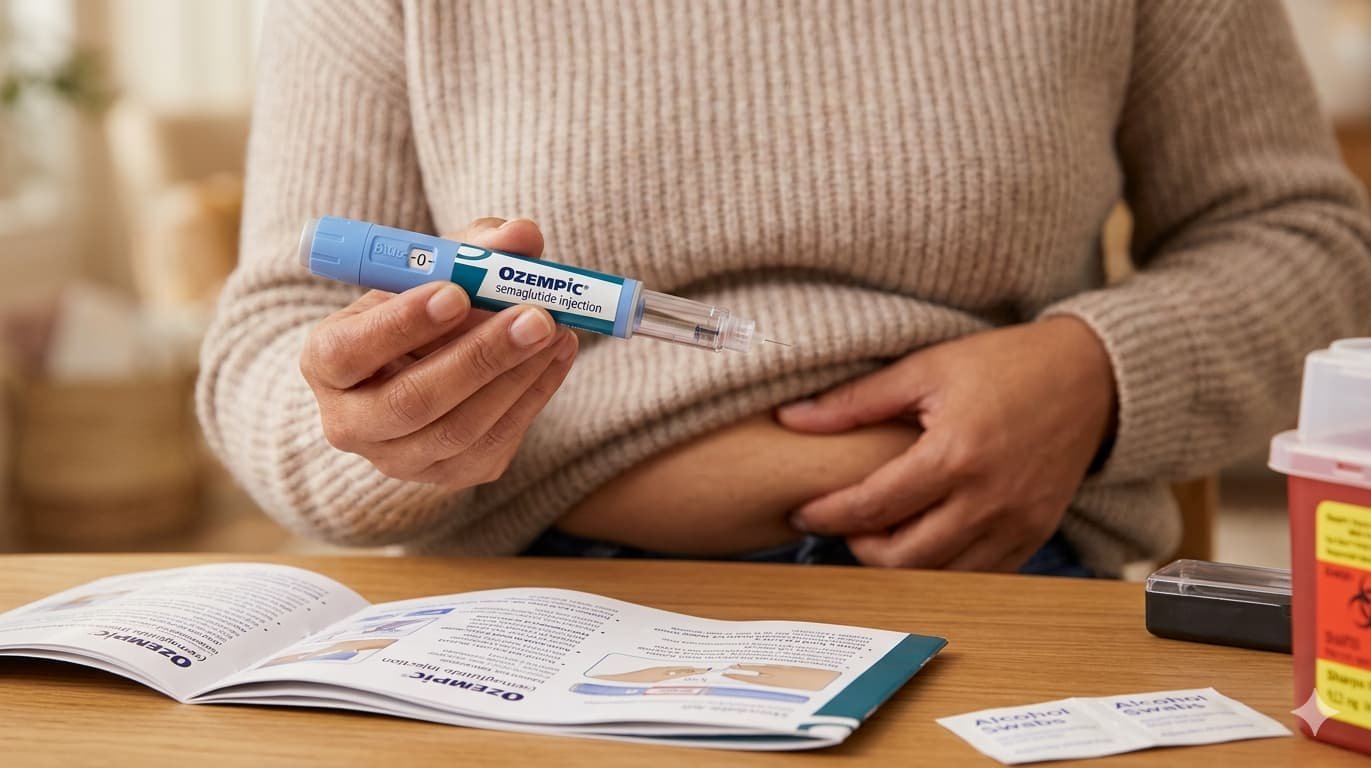
The question that has haunted every American considering Ozempic, Wegovy, or Mounjaro is the one nobody wants to ask their doctor out loud: What happens if I stop?
Clinical trials painted a frightening picture. Patients who quit GLP-1 drugs in controlled research settings regained the majority of their lost weight within 12 to 18 months — sometimes faster. The drugs, the trials suggested, worked only as long as you kept taking them. Stop the injection and watch the scale climb.
A new study published in the journal Diabetes, Obesity and Metabolism by researchers at the Cleveland Clinic has now challenged that picture directly. And the real-world answer turns out to be considerably more encouraging than the trial data suggested.
What the Cleveland Clinic Study Found
The study tracked 7,938 adults in Ohio and Florida who had been prescribed either semaglutide — sold as Ozempic and Wegovy — or tirzepatide — sold as Mounjaro and Zepbound — for between three and twelve months before stopping. Researchers monitored what treatments patients pursued after discontinuing their medication and measured how their weight changed during the following year.
The results were striking. Among patients who had been taking GLP-1 drugs specifically for obesity, the average weight loss before stopping was 8.4% of body weight. One year after stopping, they had regained an average of just 0.5% — essentially holding their results. Among patients taking the drugs for type 2 diabetes, average weight loss before stopping was 4.4% — and one year later, they had actually lost an additional 1.3% on average.
Overall, 45% of obesity patients and 56% of diabetes patients either continued losing weight or maintained their weight loss entirely after stopping their GLP-1 medication.
Why Real-World Results Differ From Clinical Trials
The difference between these findings and earlier trial data comes down to one critical variable: what patients did after stopping.
In controlled clinical trials, patients who stop a GLP-1 drug typically receive no further treatment. They are left on their own. That is not what happens in the real world — and this study captured the difference precisely.
What Patients Did After Stopping GLP-1 Drugs
| Action Taken | Share of Patients |
|---|---|
| Switched to another obesity medication | 27% |
| Restarted original GLP-1 medication | 20% |
| Pursued lifestyle care — dietitian, exercise | 14% |
| Underwent bariatric surgery | Under 1% |
| No further treatment documented | Remainder |
The patients who avoided significant weight regain were overwhelmingly the ones who did not simply stop and walk away. They pivoted — to a different drug, back to their original drug, or to structured lifestyle support with professionals. Lead study author Dr. Hamlet Gasoyan was direct about what the data shows: many patients do not abandon their obesity treatment journey when they stop one medication. They adapt. And that adaptation is what separates the real-world outcome from the clinical trial outcome.
The Conflicting Evidence — What Oxford Found
Not all recent research points in the same optimistic direction. A separate analysis from the University of Oxford, published in January 2026 and reviewing 37 studies involving more than 9,300 adults, found that weight regain after stopping GLP-1 drugs was faster than after ending behavioral programs like diet and exercise — by approximately 0.3 kilograms per month.
The Oxford analysis projected that at that rate of regain, patients who stop GLP-1 drugs without alternative support would return to their starting weight within approximately 18 months to two years.
A third study from University of Cambridge, published in eClinicalMedicine in early March, found that patients who stopped GLP-1 drugs regained roughly 60% of lost weight within one year — though the regain appeared to plateau rather than continuing indefinitely.
The three studies are not necessarily contradictory. They measure different things. The Oxford and Cambridge analyses largely track patients who stopped without structured follow-up. The Cleveland Clinic study specifically captures patients who actively pursued alternative treatments after stopping. Together, the research tells a single coherent story: what you do after stopping GLP-1 drugs determines whether you keep the weight off.
What This Means for the 15 Million Americans on These Drugs
More than 15 million Americans are currently prescribed GLP-1 medications. Millions more have tried them and stopped — because of cost, side effects, supply shortages, insurance denials, or simply because they felt they had reached their goal and wanted to stop injecting.
The Cleveland Clinic findings carry a practical message for every one of them. Stopping Ozempic or Mounjaro is not a sentence to immediate weight regain. It is a transition that requires a plan. The patients who kept their results did not keep them by accident — they kept them by switching treatments, restarting medication when needed, or building sustainable lifestyle habits with professional support.
The drugs work. Stopping them without a plan does not have to undo that work. But the plan is not optional — it is the difference between the clinical trial outcome and the real-world outcome. For anyone currently on a GLP-1 medication and wondering whether they can eventually stop, the answer the data now supports is: yes, with the right transition strategy, many people can — and do.